Updated:
by
Mohamed T. Hassan, MD, DABVLM, RPVI

Medically reviewed by Mohamed T. Hassan, MD, DABVLM, RPVI, on February 19, 2026
Non-healing wounds on the legs, ankles, or feet can be painful, slow to heal, and frightening. While some sores improve with basic care, others may indicate a more severe underlying circulation problem. Two of the most common chronic leg wounds are arterial ulcers and venous ulcers. Although they may appear similar, they develop for distinct reasons and require different treatment plans.
Understanding the difference between these leg wounds is essential for proper diagnosis, effective vein treatment, and long-term healing.
We consulted Center for Vein Restoration (CVR) vein expert Dr. Mohamed T. Hassan for clinical insight on how to identify the underlying cause of wounds affecting the leg, ankle, or foot, and to provide guidance on the most appropriate path to diagnosis, treatment, and healing.
Dr. Hassan is the lead physician at CVR vein clinic locations in Hoover (Birmingham), Alabama, and Trussville, Alabama.
To schedule an appointment with Dr. Hassan or at any of Center for Vein Restoration’s 120+ vein clinics nationwide, click below🔽

Leg ulcers develop when impaired blood flow prevents oxygen and nutrients from reaching the skin. Without adequate circulation, the skin and underlying tissues begin to break down, leading to open wounds.
Chronic wounds affect millions of people. In the United States, approximately 1–2 percent of the population will develop a leg ulcer during their lifetime. This increases to 4 percent in individuals aged 65 years and older and to 5 percent in individuals aged 80 years and older, according to the National Institutes of Health (NIH).
According to the American Family Physician Journal, most chronic leg ulcers are caused by venous or arterial disease; the majority are linked to venous reflux or obstruction, whereas about 20 percent occur in people with arterial disease, either alone or in combination with venous disease.
More than one million people in the United States suffer from venous leg ulcers. Venous ulcers are the most common type of leg ulcer, accounting for approximately 70 percent of cases. They develop when damaged leg veins allow blood to pool or become blocked, thereby increasing pressure on the skin and leading to open wounds, typically near the lower leg or ankle, per the Annals of Phlebology. Over time, fluid leaks into the surrounding tissue, damaging the skin.
Diagnosis typically involves reviewing the patient’s medical history, examining the wound and surrounding skin, and using ultrasound imaging to evaluate blood flow and vein function.
Location
Appearance
Symptoms
Because venous ulcers originate from underlying vein disease, treating the wound alone is not enough. The root circulation issue must be addressed by a vein expert.
A venous ulcer that will not heal is more than a skin issue. It is a circulation problem that requires expert care. Center for Vein Restoration’s 80+ nationally recognized vein doctors provide comprehensive diagnosis and advanced vein treatment designed to restore blood flow, relieve symptoms, and prevent recurrence. Do not wait. Early treatment leads to faster healing.
📞 Call Center for Vein Restoration at 240-249-8250
📅 Or book online HERE
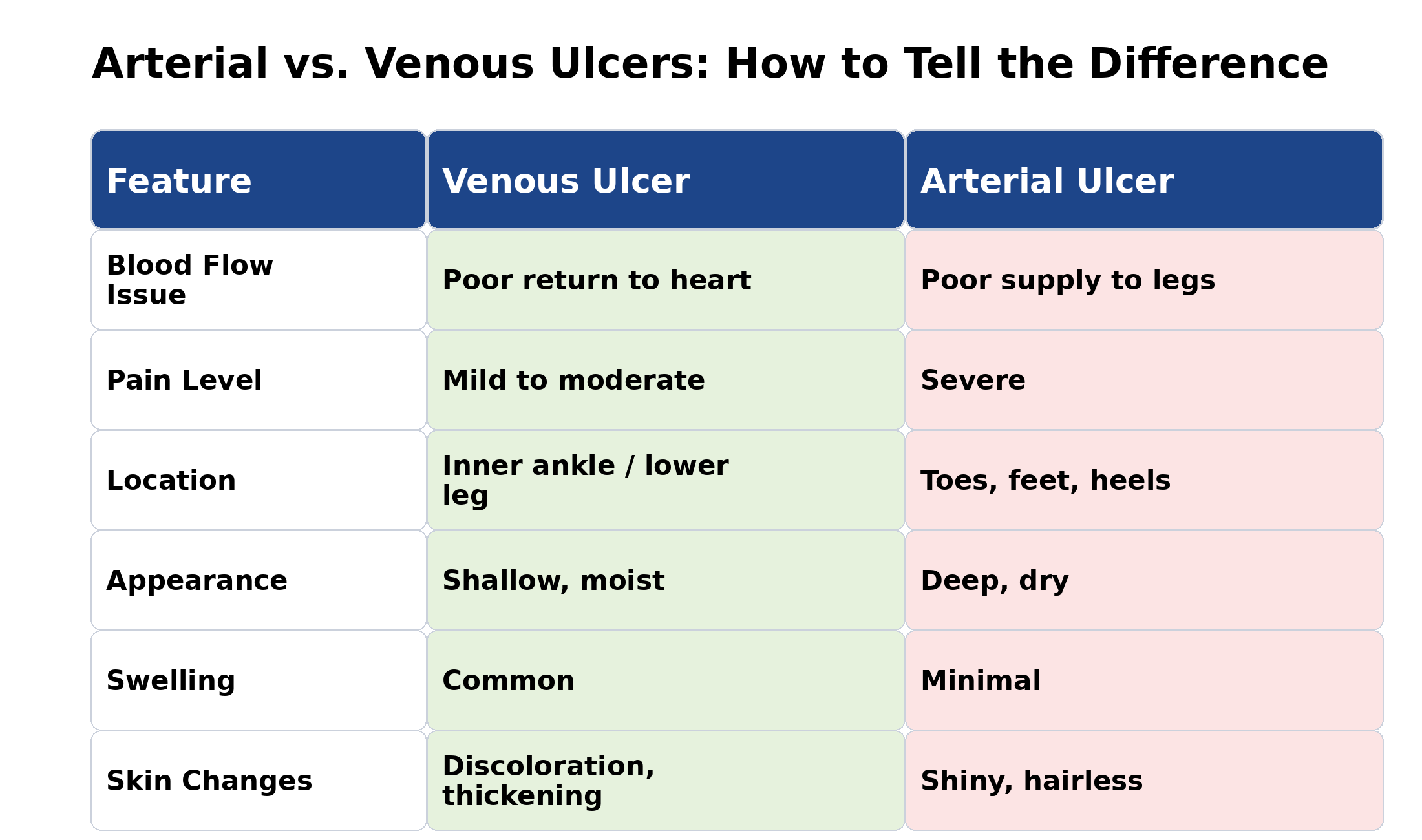
Distinguishing between arterial and venous ulcers is critical because treatments that benefit one type can worsen the other. Although both present as open wounds on the lower legs or feet, their underlying circulatory problems can lead to markedly different symptoms, wound characteristics, and healing patterns.
Venous ulcers are open skin wounds that develop when blood does not flow properly back to the heart, most often due to problems in the leg veins. Healthy veins contain small valves that help push blood upward, but when these valves become damaged, blood can pool in the lower legs. This pooling increases pressure inside the veins, a condition known as venous hypertension, which can weaken the skin and lead to ulcers, usually around the ankles, according to Johns Hopkins Medicine.
Because circulation is impaired, the body’s normal healing process slows down. Swelling, varicose veins, and chronic venous insufficiency can add even more pressure on the skin, making wounds difficult to close and more likely to return without proper vein treatment.
Location
Appearance
Symptoms
Because venous ulcers stem from underlying vein disease, healing often requires treating the primary damaged or leaky vein , not just the wound itself.
If you have a slow-healing wound near your ankle or lower leg, it may signal underlying vein disease. The vein specialists at Center for Vein Restoration use painless ultrasound and advanced minimally invasive treatments to restore circulation, promote healing, and help prevent recurrence.

Arterial ulcers, also called ischemic ulcers, are painful open wounds that form when blocked or narrowed arteries prevent oxygen-rich blood from reaching the skin, most often in the legs or feet. Poor circulation slows healing and increases the risk of infection, tissue damage, and, in severe cases, amputation, according to WebMD.
These ulcers usually appear below the ankle level, typically on the toes, feet, or heels and are often deep, dry, and well-defined. Pain can be severe, after walking few blocks or when the legs are elevated, and the surrounding skin may appear shiny, thin, or hairless, with little swelling.
Location
Appearance
Symptoms
Because blood flow is compromised, healing can be extremely slow without vascular intervention.
Because visual differences alone are not enough to diagnose the cause of a leg wound, advanced vascular testing is essential. At Center for Vein Restoration, our vein specialists use noninvasive studies, such as duplex ultrasound, to evaluate blood flow, determine whether an ulcer is venous or arterial, and develop a personalized treatment plan designed for safe, effective healing.
Leg ulcers often fail to heal because the underlying cause, most commonly poor circulation, has not been treated. When blood flow to the legs is reduced or blood pools in damaged veins, the skin does not receive the oxygen and nutrients it needs to repair itself. Conditions such as chronic venous insufficiency, peripheral artery disease, and diabetes can all slow the healing process. Infection, swelling, and repeated pressure on the wound can make recovery even more difficult.
According to the Cleveland Clinic, leg ulcers may take months to heal and can become chronic without proper care. Left untreated, they can lead to serious complications, including:
Early evaluation is critical. A Center for Vein Restoration vein specialist can identify the root cause using circulation testing and wound assessment, then create a treatment plan to improve blood flow, support healing, and reduce the risk of recurrence.
At Center for Vein Restoration, the nation’s largest physician-led vein center, specialists focus on diagnosing and treating the root causes of chronic wounds, including vein problems that contribute to leg ulcers.
Conditions we treat include:
A comprehensive vein evaluation at Center for Vein Restoration allows our board-certified vein specialists to pinpoint the cause of your symptoms and deliver a personalized, minimally invasive treatment plan designed to heal wounds, restore circulation, and prevent future complications.
👉 Book your consultation with a CVR vein specialist today and discover how simple relief can be.
Because venous ulcers originate from venous reflux and pressure buildup, treatment focuses on restoring healthy circulation.
Modern outpatient therapies, supported by vascular guidelines from organizations like the American Venous Forum, may include:
Compression Therapy
Graduated compression stockings reduce swelling and improve blood return.
Endovenous Ablation
Minimally invasive laser or radiofrequency procedures are used to close diseased veins.
Sclerotherapy
Medical injections seal malfunctioning veins.
Wound Care Management
Advanced dressings, debridement, and infection control support healing.
These outpatient treatments, performed by a board-certified vein specialist at Center for Vein Restoration, require no general anesthesia and minimal downtime.
Arterial ulcers require restoring the blood supply, not compression.
Care may involve:
Because compression can worsen arterial ulcers, accurate diagnosis is vital before starting therapy.
Not all ulcers are preventable, but managing underlying risk factors and circulation health can significantly reduce the likelihood of developing one.
Tips to Prevent Ulcers
Research shows that treating circulation problems early can speed wound healing and reduce recurrence risk. A landmark randomized trial published in the New England Journal of Medicine found that early vein treatment led to faster healing and longer ulcer-free periods.
Seek medical care if you notice:
A prompt evaluation by a vein specialist ensures accurate diagnosis and faster healing. Learn how to prepare for your consultation HERE.
If you are living with a non-healing leg wound, do not wait for symptoms to worsen. Schedule a comprehensive vein evaluation at Center for Vein Restoration, where our board-certified specialists use advanced diagnostics and minimally invasive treatments to restore circulation, accelerate healing, and help prevent ulcers from returning.

1. How do I know if my leg ulcer is venous or arterial?
Venous ulcers usually appear near the inner ankle and are often accompanied by swelling, heaviness, and visible varicose veins. Arterial ulcers typically occur on the toes or feet, are deeper and more painful, and are associated with poor arterial blood flow, which must be confirmed by vascular testing.
2. Are leg ulcers dangerous if left untreated?
Yes. Without treatment, leg ulcers can become infected and may lead to complications such as cellulitis, bone infection, tissue death, or even amputation in severe cases.
3. How long does it take for a leg ulcer to heal?
Healing time varies based on the cause and severity of the ulcer. With proper circulation treatment and wound care, some ulcers heal within weeks, while others may take several months.
4. What kind of doctor treats leg ulcers?
A vein specialist or vascular physician evaluates circulation problems that cause many chronic leg ulcers. These experts use ultrasound and other tests to diagnose the underlying condition and recommend targeted treatment.