10 Myths About Venous Insufficiency
“Vein treatments are for cosmetic concerns only.” Often thought as a cosmetic nuisance, varicose veins represent an underlying venous disease that
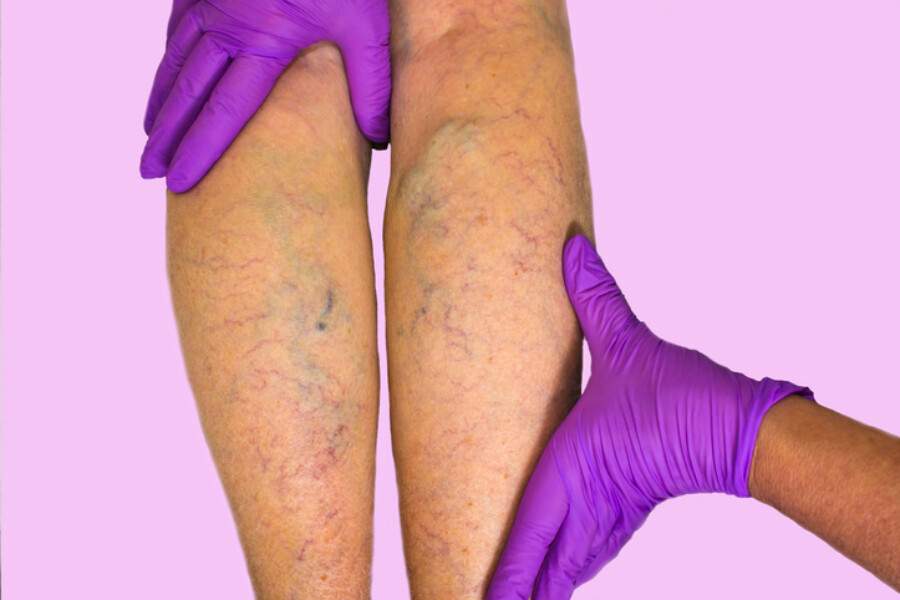
Maybe you’ve heard “chronic venous insufficiency” and “chronic venous stasis” used interchangeably. That’s because both terms refer to the same vascular disorder.
Chronic venous insufficiency (CVI) refers to a number of conditions related to abnormal blood flow in the legs veins. Chances are, you’ve also heard of the term “chronic venous stasis'' and wondered how it relates to chronic venous insufficiency or whether it’s a completely different medical diagnosis. Actually, chronic venous insufficiency and chronic venous stasis are two names used interchangeably for the same vascular condition. Within this article, we will refer to both as CVI.
Arteries and veins regulate normal blood flow. Arteries pump oxygen-rich blood from the heart to your organs and tissues. The deoxygenated blood returns to the heart with the help of valves in the leg veins. For various reasons, the valves can weaken, causing blood to backflow into the vein and leading to CVI. Although CVI is frequently associated with varicose veins, it causes other vascular issues, as well.
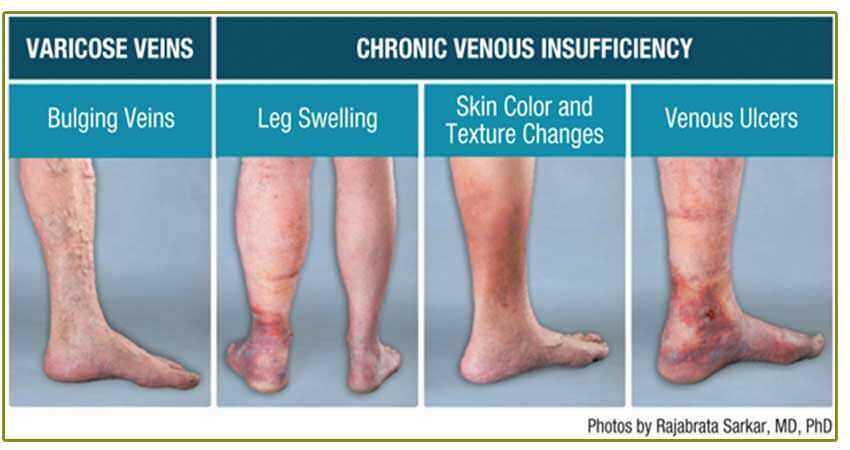
Perhaps the most visible sign of CVI is varicose veins. As blood pools in the veins, the vein walls stretch to the point where swollen, twisted varicose veins appear on the legs and feet. However, varicose veins aren’t the only indication of poor circulation or CVI.
Beyond protruding veins, CVI symptoms range from leg pain and heaviness to cramping, particularly after sitting for long periods. CVI can also cause changes in skin texture and color.
As blood pressure builds within the veins, tiny blood vessels or capillaries burst. This leads to flaking, itchy, and reddish-brown skin that’s also sensitive to the touch. As more blood vessels burst, the tissues become so inflamed that open sores can develop. These sores can be difficult to treat and may lead to further infection.
CVI is also linked to a clotting condition known as deep vein thrombosis (DVT). Slow-moving blood in the leg veins increases the risk of clots forming. These clots may then break away and lodge themselves in the lungs. A clot in the lung deprives the lungs of oxygen, leading to a potentially life-threatening pulmonary embolism. After a clot is resolved, some people develop CVI or post-thrombotic syndrome. In some instances, pelvic tumors or malformations in the veins can cause CVI.
Certain factors put you at greater risk for CVI. These include:
Gender. CVI is more common among women due to hormonal changes during pregnancy and menopause. These hormones increase blood flow and dilate the veins, which encourages blood to pool.
Heredity. If a close family member has varicose veins or other CVI symptoms, you are more likely to experience the same condition due to genetics.
Weight. Being overweight strains your veins, increasing the likelihood the valves will weaken and lead to CVI.
Sedentary Lifestyle. Those who sit or stand for long hours — or don’t have a regular exercise routine — are at risk of developing CVI. A sedentary lifestyle hinders proper blood flow, allowing blood to become stagnant within the vein. Even sitting for a long trip on a plane or car can increase the risk of CVI.
Age. As we age, the vein valves lose elasticity. Weakened valves cannot push blood back to the heart, so blood pools within the veins.
Your veins specialist will conduct a physical examination and perform a duplex or vascular ultrasound to diagnose CVI. During the ultrasound, a hand-held device applied over the legs sends out sound waves. The waves bounce off the veins and create an image of how the blood flows through the veins.
CVI can be treated with both surgical and non-surgical methods. You may find relief from wearing compression stockings that support blood flow in the legs or by elevating your legs for 30 minutes a day.
CVI can advance and develop into varicose veins that are painful and unsightly. Luckily, there are minimally invasive office procedures that can restore proper blood flow. These include sclerotherapy, a procedure that uses a safe solution to close the diseased vein. Endovenous thermal ablation is another option. The heat from laser or radiofrequency waves irritates the vein walls, so they seal shut. Eventually, the varicose vein is reabsorbed by the body as blood diverts to healthier veins.
For slow-healing leg sores caused by CVI, an Unna Boot wraps the wound in several layers of compression soaked with a zinc oxide gel. If infected, you may be prescribed antibiotics. If you’ve been diagnosed with DVT or post-thrombotic syndrome, your doctor may prescribe medication to prevent another clot.
CVI, or chronic venous stasis, is a progressive disease. However, simple lifestyle changes can slow or prevent the condition. Maintaining a healthy weight reduces the stress on your veins. Likewise, exercising regularly supports proper blood flow, especially when you’re engaging the calf muscles. When working the calf muscles during activities such as biking or walking, the muscles massage the veins to help push blood through the veins.
Center for Vein Restoration physicians focus their practice solely on treating vein disorders. We offer state-of-the-art diagnostic techniques and therapies to relieve you of the pain caused by varicose veins and CVI. Find a location close to you and book your appointment today!