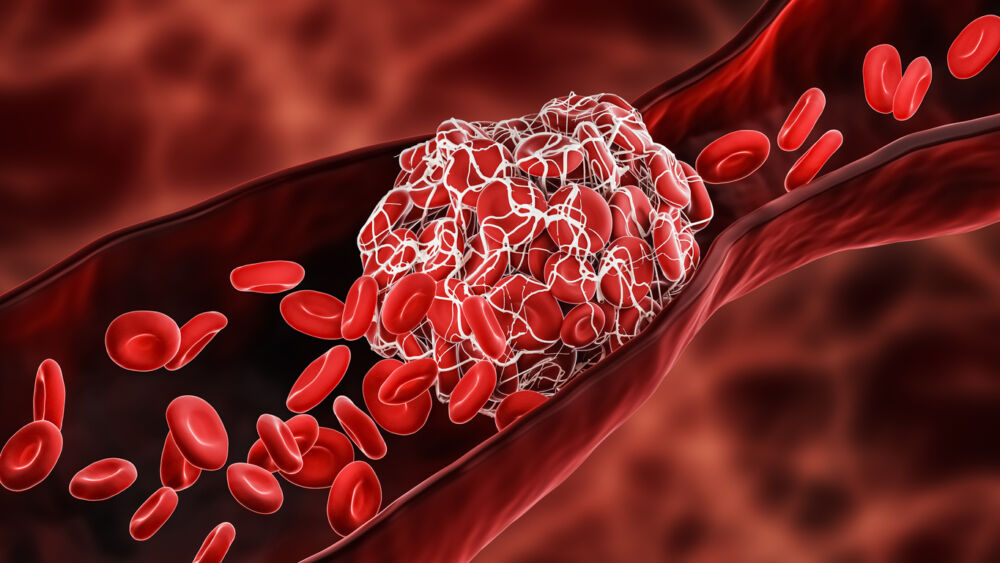
How To Check for DVT At Home
Deep Vein Thrombosis are a potentially life threating medical condition. Here are some of the symptoms of a DVT to be aware of and a quick test you can do at home.
Laura Kelsey, MD, is board-certified in general surgery and specializes in diagnosing and treating vein disease. She is the lead physician at Center for Vein Restoration center locations in Grand Rapids, MI, and Norton Shores, MI. She is a sought-after expert presenter at international meetings about deep venous thrombosis (DVT) and is an authority on blood coagulation, prevention, and the treatment of other venous disorders.
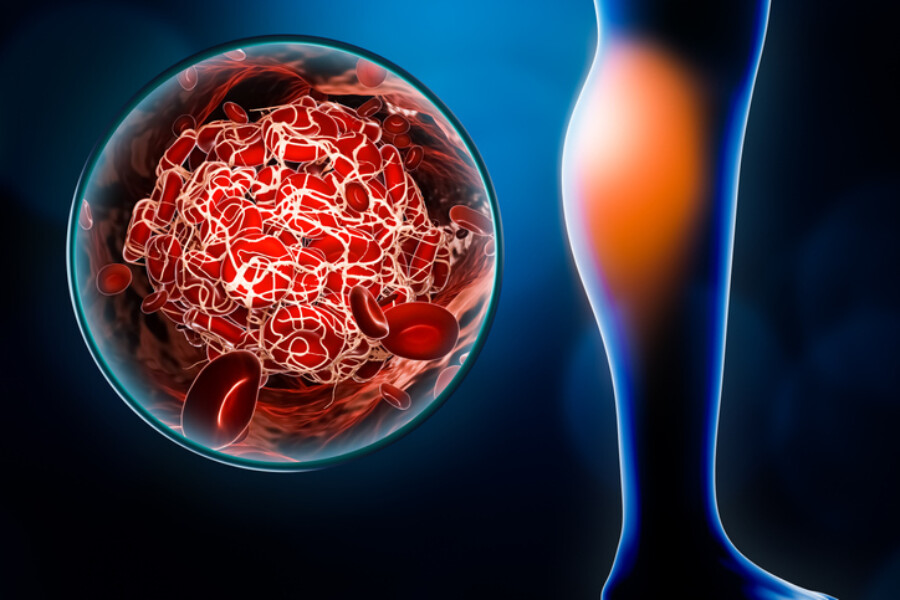
Center for Vein Restoration (CVR) vein disease doctor Laura Kelsey, MD, explains that deep vein thrombosis (DVT) occurs when a blood clot (thrombus) forms in a vein deep to the muscle, causing circulation to be partially or completely blocked. The blocked flow of blood can cause pain and swelling in the affected leg, as well as warmth, redness, and soreness to the touch, and cramping. Deep vein clots can also form in the pelvis and arms, but this occurs far less often.
A DVT blood clot can break off and travel through the bloodstream and into the lungs, leading to a blockage in one of the pulmonary arteries. This is otherwise known as a pulmonary embolism. (PE), the blocked blood flow to the lungs can be life-threatening. Immediate treatment can reduce the risk of death from a PE.
Dr. Kelsey adds that the term venous thromboembolism (VTE) Includes both deep vein clots (DVT) and clots that go to the lungs (PE). Annually, approximately 1 per 1,000 adults will experience a DVT.1 The Centers for Disease Control and Prevention (CDC) estimates that up to 100,000 Americans die every year from DVT/PE. Sudden death is the first symptom in about 25 percent of people who have a PE. About one-third to one-half of those who have experienced a DVT will have long-term complications (known as post-thrombotic syndrome) such as swelling, pain, discoloration, and scaling in the affected limb.2
There are many possible causes for blood clots, says Dr. Kelsey. These include:
According to Dr. Kelsey, only about 5 to 12 percent of patients with isolated calf vein clot patients have symptoms. Some patients do not realize that they have a clot until they develop leg pain or swelling. This usually occurs when the clot travels up their leg from the calf.
She explains that clots usually start small in the calf. Over the next 1- 2 weeks, the clot has the opportunity to grow up the leg and / or travel (i.e., move to the lungs). The higher the clot travels up the leg toward the pelvis, the more symptoms patients will have. This is because the higher the clot, the more the blood flow out of the leg is affected. A “traffic jam” develops the person experiences pain and swelling.
Pain or swelling should be considered a medical emergency, especially after a provoking event such as surgery, a long plane or car ride, or after starting birth control.
CVR offers a same-day DVT service to patients whose doctor suspects are experiencing a blood clot. During this appointment, patients receive a thorough full-leg ultrasound, including the calf veins. If the patient is asymptomatic and the clot is far away from the knee, the patient can be put “observation.” That is, given baby aspirin and checked regularly with Ultrasound throughout the clot growth phase, about 14 days.
If there is an isolated calf vein clot that is symptomatic, or close to the Popliteal vein (large vein behind the knee), anticoagulation (blood thinners) is prescribed.
If the clot was “provoked” by surgery or another event, the patient typically would be put on blood thinners for three months. If the clot was “unprovoked” and the cause is unknown, the risk of recurring blood clots is higher than in patients that have an event causing the clot. In these circumstances, the risk of bleeding needs to be compared to the risk reduction in clotting. Aspirin can also be used following clots to reduce the risk of recurrence. o. The patient must have the risk and benefits of staying on blood thinners constantly monitored by their physician.
Patients can have a filter placed in the Vena Cava (the major vein in the abdomen that brings blood back to the heart) if a patient has a known clot and cannot take blood thinners. There are permanent and retrievable filters that catch clots and prevents them from traveling to the lungs. These are placed to help reduce the likelihood of death from a massive PE to the lungs.
In addition to reducing controllable risk factors, Dr. Kelsey also suggests that anyone concerned about their risk of DVT take a free online self-assessment. For example, the Caprini Risk Score for Blood Clots assigns a point value to each risk and helps people understand their personal risk.
Dr. Kelsey encourages people to discuss their assessment score with their physician, especially if blood clots run in the family. In Dr. Kelsey’s practice, if a patient presents with a blood clot, she first “gets them calm and gets them safe by treating the blood clot.” At the follow-up appointment, Dr. Kelsey discusses ways of reducing blood clot risk long-term and the risk to their family members.
“Awareness and being proactive is the name of the game when it comes to DVT and blood clot prevention.” - Laura Kelsey, MD
We can help you avoid a long and costly trip to the emergency room by providing thorough, efficient, same-day DVT management. Call 177-SCAN-DVT for more information or to schedule an appointment. Treatment is covered by most major insurance providers, including Medicare and Medicaid.