Updated:
by
Swapna Anandan, MD, FACP, DABVLM

Medically reviewed by Swapna Anandan, MD, on December 12, 2025
Many patients first learn about May-Thurner syndrome (MTS) after experiencing unexplained leg swelling, heaviness, or even a deep vein thrombosis (DVT) in the left leg. As more people become aware of the condition, one question keeps coming up: Is MTS hereditary? Understanding whether family history influences your risk is an integral part of protecting long-term vein health.
The short answer? Current research has not proven that MTS is hereditary, but some families do seem to share similar vein anatomy. This means genetics might play a small role, but experts are still studying how strong that connection may be.
In this blog, Swapna Anandan, MD, lead vein physician at Center for Vein Restoration (CVR) clinics in Bloomfield, CT, and South Windsor, CT, takes a closer look at what MTS is, whether it may run in families, the symptoms to watch for, and how vein specialists treat the condition.
If you experience new or recurring left-leg swelling, heaviness, or discomfort, Center for Vein Restoration (CVR) can evaluate you for MTS and provide answers you can trust. Call 240-249-8250 to schedule an appointment.
📅To schedule an appointment at CVR in Bloomfield, CT, CLICK HERE
📅To schedule an appointment at CVR in South Windsor, CT, CLICK HERE
📍To schedule an appointment at any of CVR’s other 120+ vein clinics nationwide, CLICK HERE
📞Call Center for Vein Restoration Patient Services at 240-249-8250

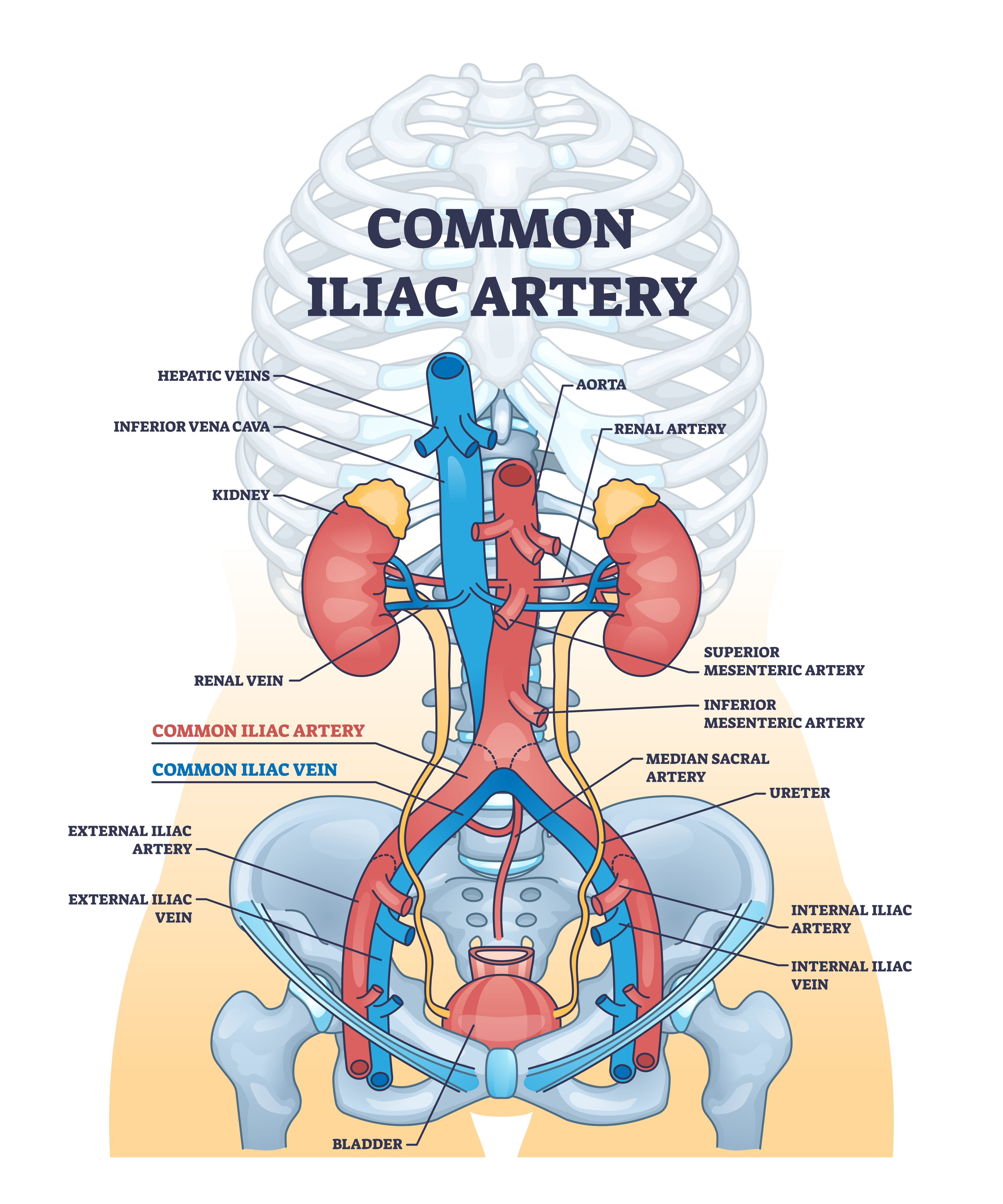
MTS occurs when the right iliac artery presses against the left iliac vein, narrowing the vein and slowing blood flow from the left leg back to the heart. Over time, this reduced flow can irritate the vein and increase the chance of developing a DVT. Many people have this compression for years without noticeable symptoms, and sometimes it only becomes apparent once swelling or a blood clot forms.
According to the National Library of Medicine, MTS symptoms usually affect the left leg since the condition impacts the left iliac vein. Patients may notice:
Persistent symptoms on the left side, especially those that recur or worsen, should be evaluated by a vein specialist.
Certain factors can make existing vein compression more noticeable or more likely to cause symptoms. These include:
Note that these factors don’t cause MTS; they can aggravate symptoms in someone who already has pelvic vein compression.
If you have risk factors and ongoing left-leg symptoms, a vein specialist can provide clarity and support. Book a consultation with CVR by calling 240-249-8250 or clicking the button below.

Without treatment, vein compression can lead to significant circulation issues, such as:
Recognizing MTS symptoms early can reduce the likelihood of these long-term complications.
Researchers haven’t identified a single gene that directly causes MTS, and it isn’t considered a strictly hereditary condition. Most cases result from anatomical differences in pelvic structure that are present from birth but don’t follow a clear genetic pattern.
However, some families share physical traits such as pelvic anatomy, vein compressibility, or inherited clotting tendencies. These traits may increase the likelihood of developing MTS or related complications. A family history of unexplained leg swelling, pelvic vein issues, or recurrent DVTs can be helpful information to share with your specialist.
If you have a family history of venous disease and experience left-leg symptoms, a consultation can help determine if MTS may be a factor.
Treatment for MTS focuses on restoring healthy blood flow, easing symptoms, and lowering the risk of future DVTs. Options may include:
Your treatment plan will be tailored to your symptoms and long-term vein health goals.
MTS can’t be entirely prevented because it stems from natural anatomy. Patients can lower the chance of complications and encourage healthy circulation by:
These steps support smoother, healthier circulation, even when veins are being put under pressure.
MTS isn’t considered hereditary, although some family traits may increase the likelihood of vein compression or clotting. Many people have MTS without realizing it until symptoms appear. Recognizing early changes in the left leg and seeing a vein specialist can help protect long-term circulation and reduce complications.
If you have ongoing left-leg swelling, discomfort, or a history of DVTs, CVR can help determine whether MTS is the cause. Our board-certified vein specialists also offer minimally invasive treatment options to restore proper blood flow and relieve symptoms.
📞 Call Center for Vein Restoration at 240-249-8250
📅 Or book online HERE

1. Can May-Thurner syndrome affect the right leg?
MTS almost always affects the left leg because of how the iliac artery and vein cross in the pelvis. Actual right-sided cases are extremely rare and usually involve different anatomical variations. If swelling or discomfort appears on the right side, another vein condition is usually responsible.
2. How common is May-Thurner syndrome?
According to Cleveland Clinic, about one in five people has iliac vein compression. Still, many aren’t formally diagnosed with MTS because it usually doesn’t cause symptoms unless a DVT develops.
3. Can May-Thurner syndrome cause pelvic pain?
Some patients experience pelvic pressure or discomfort because the compressed vein can create higher pressure in the pelvic region. This is more common in people who spend long periods sitting or who have additional pelvic vein conditions. Persistent or unexplained pelvic pain may warrant a specialist evaluation.
4. Can younger adults or teens have May-Thurner syndrome?
Yes. MTS is based on anatomical factors, so it can be present from childhood, even though symptoms often appear later. Teenagers and young adults may notice swelling or heaviness during growth spurts, sports activities, or long sitting periods. Any persistent one-sided leg symptoms should be assessed.
5. Does weight affect the severity of May-Thurner syndrome?
Body weight doesn’t cause MTS, but extra abdominal pressure can make vein compression more noticeable. Some patients report increased swelling or discomfort with higher body weight. Gentle activity and movement breaks often help relieve pressure and boost circulation for people with MTS.
