Updated:
by
Sanjiv Lakhanpal, MD, FACS

Hi, my name is Sanjiv Lakhanpal, and I am a cardiovascular surgeon and also the president and CEO of the Center for Vein Restoration. Today, I will be talking to you about the venous disease in a nutshell.
With every beat of the heart, 75 milliliters of blood is pumped into the body generating a cardiac output of 5 liters per minute. This blood is taken to the ends of our body through the arterial system. From the far reaches of our body, blood is brought back to the heart against a gravitational pressure of greater than a hundred millimeters of mercury through an elegantly designed system of veins. These veins can be divided into the Superficial Veins, the Deep Veins, and the Perforating Veins. The Superficial Veins are the ones that lie superficial to the Muscular Fascia. The Deep Veins are the ones that lie deeps to the Muscular Fascia, and the Perforating Veins are the ones that perforate through the Muscular Fascia. In addition, the Reticular Veins are the ones that lie in the sub Dermis layer, and the Spider Veins are the ones that lie in the Dermis layer.

The venous system needs to be evaluated as a single continuous system. This system starts from the Dorsum of the feet through the legs into the abdomen and pelvis, the subdiaphragmatic venous areas, and finally into the chest and the heart. Let us now look at this entire interconnected system of veins. From the Dorsum of the foot, superficial veins continue on the medial side as the Great Saphenous veins. On the lateral side as the Small Saphenous Veins. These veins drain respectively into the Femoral and the Popliteal Veins. They usually paired deep veins of the leg, follow the arteries, also taking on their names. Blood travels back to the heart through the Femoral Vein, the External Iliac Vein, Common Iliac Vein, and finally, the Inferior Vena Cava.
It is the left Ovarian Vein that drains into the left Renal Vein. The Intrapelvic and the Extrapelvic Veins communicate through a rich network of connecting veins.
In the standing position, blood has to travel back up to the heart against a pressure gradient of over a hundred millimeters of mercury. To facilitate that, nature has to come up with a system of ingenious mechanisms.
One such mechanism involves strategically-placed anatomical enhancements that prevent blood from falling down a certain column. These enhancements are called Venous Valves. The closer we are to the ground in our standing state, the higher the gravitational pull, and to counter that, the more numerous are the valves.

The second, probably even more important mechanism, is the blood pumping action of the calf muscle when we walk. Remember, as I just mentioned, blood has to travel back to the heart against a pressure gradient. To facilitate this arduous journey, the calf muscle pump is recruited to work when we walk. This pump propels blood away from the feet, causing the venous pressure in the foot to drop below 30 millimeters of mercury when we walk.
If this ambulatory venous pressure fails to drop below 30 millimeters of mercury, the condition is called Ambulatory Venous Hypertension.
Ambulatory Venous Hypertension in the lower extremity occurs in patients with valvular reflux or venous obstruction. Either in the legs or the pelvis through the Escape veins.
This ambulatory venous hypertension is what changes the hemodynamic balance at the capillary level, causing tissue changes that lead to the signs and symptoms of venous insufficiency in the legs.
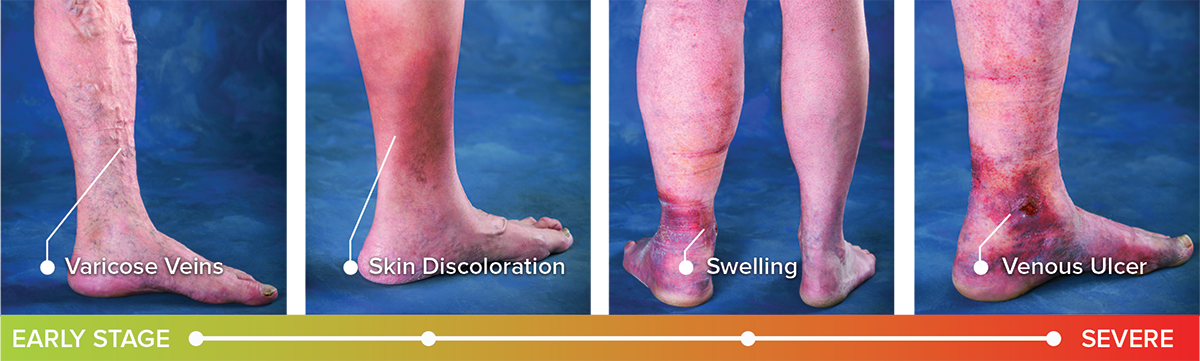
These clinical presentations of venous insufficiency are classified by the CEAP. C.E.A.P classifications.
If venous hypertension stays contained within the pelvis, that leads to pelvic congestion syndrome. These devastating symptoms of pelvic congestion include chronic pelvic pain lasting for more than six months, heaviness in the groin and Belvoir areas, and painful intercourse.
If the patient presents with purely cosmetic symptoms as spider veins, these veins are treated with sclerotherapy or laser treatments only.
In patients with more advanced venous insufficiency, the entire infra diaphragmatic venous system needs to be evaluated. This will tell us what part of their system actually needs to be treated if the cause of the leg symptoms is Venous reflux in the superficial veins of the lower extremity. In that case, the refluxing vein is closed through various modalities, and blood is rerouted through a healthy vein.

While of the cause of the leg symptom is Venous hypertension in the pelvis and blood is leaking into the lower extremity through Escape veins than to treat varicose veins in the legs, it is venous hypertension in the pelvis that needs to be treated first Venous hypertension in the pelvis without adequate escape veins may lead to pelvic congestion syndrome. In that case, the cause of this pelvic hypertension could either be iliac vein obstruction, as in Mae Turner syndrome or ovarian vein reflux. The obstruction is treated with a stent while the ovarian vein reflux is treated by embolizing the refluxing vein shut.
So now you realize that when you seek attention for your venous insufficiency in the legs, a complete evaluation of the entire venous system needs to be done, and not infrequently, the challenge may be in addition to the legs also in the abdomen or the pelvis. Consequently, your physician may choose to do more than just treat the legs to get the right treatment option to you.
Center for Vein has over 90 locations across the United States. If you are experiencing venous problems, we are here to help! You can get started easily by scheduling a consult through our online system.