Should vein health be a consideration during long travel?
"Yes, absolutely," says Dr. Kasinadhuni, "vein health should be a strong consideration during long travel" because being sedentary can negatively impact vein health. He explains that while most people have heard of blood clots or deep vein thrombosis (DVT) relating to travel, few understand how blood clots can impact a person's overall health and well-being.
Dr. Kas assures that long trips can be safe and carefree if travelers prioritize vein health and take a few simple precautions.
But not all travel is created equal.
What Types of Travel Poses Health Risks?
Dr. Kas points out that millions of Americans drive or ride in cars or hop on a train or bus daily, yet we don't hear of people forming a dangerous DVT blood clot every day. As data suggests, prolonged, sedentary travel over four to six hours at a time or more causes blood clots to form.
A DVT blood clot develops in the deep veins of the thigh or lower leg when blood is prevented from flowing freely and pools in the blood vessels.
What are the possible health risks of long plane travel?
According to the Centers for Disease Control and Prevention (CDC), More than 300 million people travel on long-distance flights (generally more than four hours) each year. The following are blood clot risks that these far-flung travelers should be aware of:
- Decreased oxygen pressure in an airplane cabin while flying can contribute to blood clotting.
- Dehydration is an often overlooked and far too common a risk during travel, says Dr. Kasinadhuni. A lack of fluids can cause blood vessels to narrow and blood to thicken. The Aerospace Medical Association (AsMA) recommends drinking more than a cup of water every hour while on a plane and increasing hydration before getting to the airport.
- Sitting for a prolonged time with your knees at an angle can hinder blood flow.
Other risks factors of long plane travel include:
- Being over the age of 40
- Being female
- Using estrogen-containing birth control
- Being pregnant or recently post-partum
- Obesity
- Cancer or recent cancer treatment
- Preexisting vein disease
- Previous blood clot or a family history of blood clots
- Recent immobility or injury (within three months)
Dr. Kas recommends that if you have any of these risk factors and are concerned, have a conversation with your physician or vein specialist about taking these precautions before long plane travel. The doctor may recommend taking aspirin or blood thinner to help offset these risks in some cases.
What are the symptoms of DVT?
DVT
can lead to pulmonary embolism (PE). This is when a blood clot, usually from the leg, breaks loose and travels to the lungs, blocking blood flow. If diagnosed and treated early, one can survive a PE. If left untreated, a PE can cause heart damage or be fatal. If you experience these symptoms during travel or other times, you must seek immediate medical attention.
Symptoms include:
- Swelling, pain, or tenderness in the affected limb (usually the leg)
- Unexplained pain or tenderness
- Skin that is red and warm to the touch
What can I do to prevent blood clots during long travel?
Walking
Dr. Kasinadhuni advises that the most crucial thing you can do during travel is to get up and walk as much as possible. He recognizes that walking is impossible during certain modes of transportation, however. For example, it is easier to stand and walk on a bus, train, or plane than in a car.
For car travel, Dr. Kas recommends stopping every one to two hours to get out and walk for five minutes. He explains why this is important: walking activates calf muscles, which act as a pump, pushing venous (vein) blood back toward your heart. "When activated, the calves are responsible for a significant portion of venous circulation. When you're walking, venous circulation drastically improves, which can largely prevent blood clots' development," implores Dr. Kas.
Compression stockings
"Compression stockings are the gold standard for managing vein disease and greatly reduce the incidents of blood clots," says Dr. Kasinadhuni.
How often should someone stand during travel?
Dr. Kasinadhuni calls it a "misconception" that merely standing during long travel is enough to prevent blood clots. When you stand, the blood in the vein naturally gets pushed down due to gravity and can pool in the veins. This blood stagnation is called venous stasis, which causes swelling of the legs and ankles and feelings of heaviness, aching, or tiredness.
"When blood sits and coagulates, it is the perfect condition for a blood clot," says Dr. Kas. He adds that activating the calf muscle by walking or other calf exercises is the key to preventing blood clots, not just standing.
Tips for activating the pump action of calf muscles while traveling
Whenever possible, walk. However, if you find yourself in a crowd or otherwise unable to walk for an extended length of time, there are exercises you can perform to get your blood circulating:
Standing toe raises. Elevate to the point where the balls of your feet are off the ground, activating the calf muscles. Do this ten times. Give yourself a 15-30 second break and repeat two to three times. Repeat every half hour to an hour if walking is not possible.
Seated toe raises. If you're confined to a seat; with feet on the floor, lift your toes then lift your heels. Continue for 30 seconds.
Ankles circles. Raise your leg and hold your ankles stationary. Draw "circles" in the air with your feet.
Knee lifts. Put your hands on your thighs and lift your knees one at a time to your chest while contracting your thigh muscle. Do these five to 10 times and repeat every half hour to an hour.
Dr. Kasinadhuni's tips for people who have symptoms of vein disease
"If you have varicose veins or other symptoms such as leg swelling, aching, and throbbing, the best tip I can give is to see a vein specialist," recommends Dr. Kas. He says that a person with chronic venous insufficiency is at increased risk of developing DVT. These incompetent veins are more prone to venous stasis that can turn into blood clots.
See a vein specialist before you travel
CVR has over 100 clinics across the United States. Dr. Kas says that anyone concerned about their vein health can have a free brief evaluation or a more comprehensive consultation with a physician.
Schedule online
or call 240-965-3915 to speak with a live patient services representative who can answer your questions and schedule with a board-certified vein physician near you.

 About Vein Disease
About Vein Disease
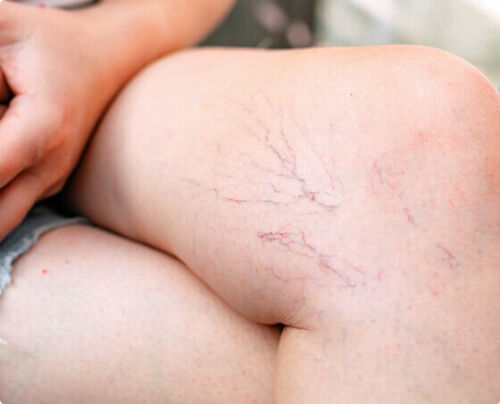 Spider Veins
Spider Veins
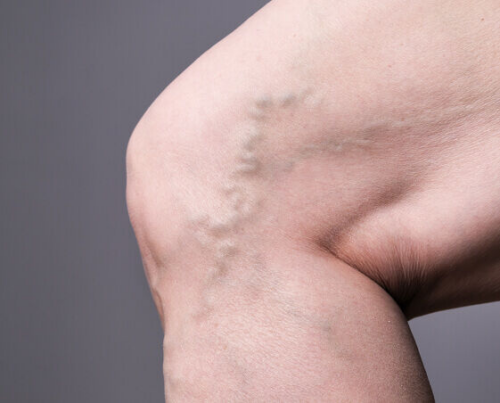 Varicose Veins
Varicose Veins
 Vein Disease Treatments
Vein Disease Treatments
 Treating Spider Veins
Treating Spider Veins
 Treating Varicose Veins
Treating Varicose Veins
 About Us
About Us
 Patient Resources
Patient Resources
 Physician Resources
Physician Resources


